Treating keratoconus based on research, not intuition
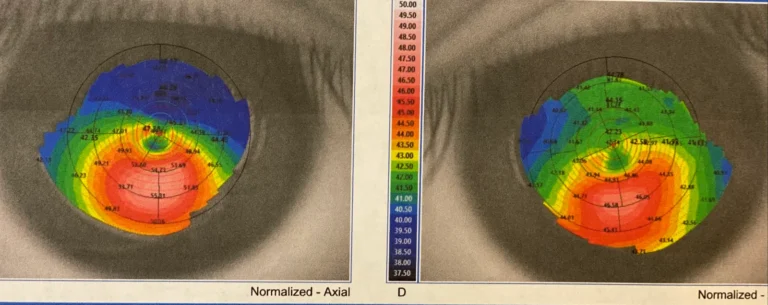
Suspecting a case of undiagnosed keratoconus, I performed a corneal topography scan on her eyes. The scan confirmed a case of moderate bilateral keratoconus. Showing the patient, the 3-D scans of her cone-shaped cornea (the clear part of the eyes), I said gently, “I’m afraid that you have keratoconus in both eyes, that may be the main reason is why you have been having all these vision issues”.
Facing such inappropriate and unexpected reactions, I was taken aback, but then I understood and sympathized with her. The relief of finally knowing what was wrong with her eyes after all these years momentarily overcame the natural apprehension and worries of receiving such unwelcome news.
Another way eye doctors treat keratoconus is using a procedure called corneal cross-linking to achieve the same type of cornea stiffening.
“I can see light at the end of the tunnel, and it isn’t a train.” – David Bowie.
If you make it here, you are probably depressed by now. Fortunately, there is a light at the end of the tunnel, and it is a UV light. In 2016, the FDA finally approved a surgical procedure called corneal cross-linking as a treatment for keratoconus, to the delight of keratoconus-enthusiast eye doctors everywhere. Corneal cross-linking (CXL) has been available in Europe for years prior to FDA approval in the US.
The procedure takes less than an hour, involving soaking your eyes with specialized vitamin B-12 eye drops, and then shining UV lights on them to create more cross-collagen bonds, thus making your eyes stronger which in turn slow down keratoconus progression.
The procedure has a success rate of more than 90%. [11] Put it simply, it is the best way we have today as of 2021 to significantly slow or even stop keratoconus from getting worse. Here is a short video of a patient undergoing a corneal cross-linking (CXL) procedure.
Corneal cross-linking is especially important in those patients that have 20/20 in one eye and “bad vision” in the other eye as mentioned above. Think about it. If you already have one bad eye, and the remaining eye is good, for now, your priority should be keeping the good eye from getting worse like the “bad” one.
Another important consideration is your age when corneal cross-linking is considered as a treatment option. Research showed that keratoconus is often more severe at the time of diagnosis when compared to adults, and in the case of progression, they also progress faster than adults [12]. Thus, it is most critical that once a proper diagnosis is made in children, corneal cross-linking or CXL should be the first treatment method for consideration.
At the time of this writing, December 2021, the FDA has approved only one cross-linking platform for the treatment of progressive keratoconus in patients older than 14 years of age: the iLink corneal remodeling platform (Glaukos). The platform consists of Photrexa Viscous (riboflavin 5’-phosphate in 20% dextran ophthalmic solution), Photrexa (riboflavin 5’-phosphate ophthalmic solution), and the KXL system, approved in 2016[11].
Insurance coverage varies depending on your plan coverage. It’s important to find out exactly what your insurance pl. covers before proceeding with corneal cross-linking. Paying attention to the enrollment window of your health insurance plan may allow you to change to a better coverage plan that could potentially save money on the procedure.
In San Diego where I practice keratoconus and myopia management, the typical price for corneal cross-linking for uninsured patients is around $6000 per eye, as of December 2021.
Keratoconus is a bilateral and progressive eye condition, usually starts during high school years and stabilizes around the early forties. There are multiple treatments available, but the best treatment for keratoconus usually involves corneal cross-linking (CXL) for vision stabilization and scleral contact lens wear for vision rehabilitation. Early diagnosis and intervention are the keys to successful management of the disease.

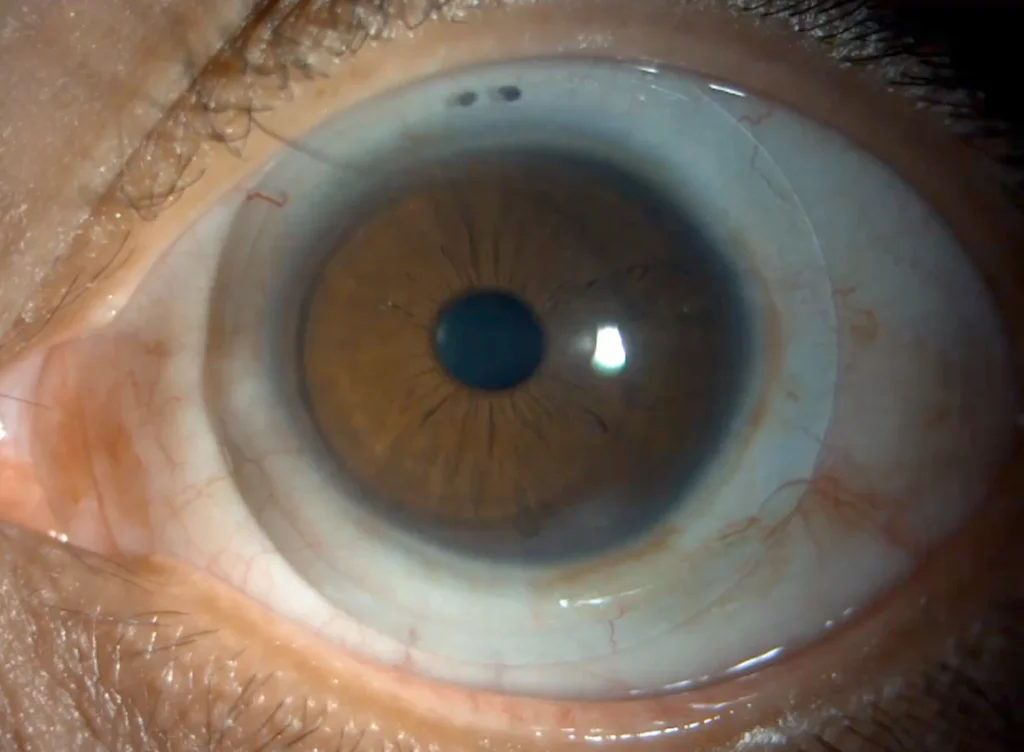
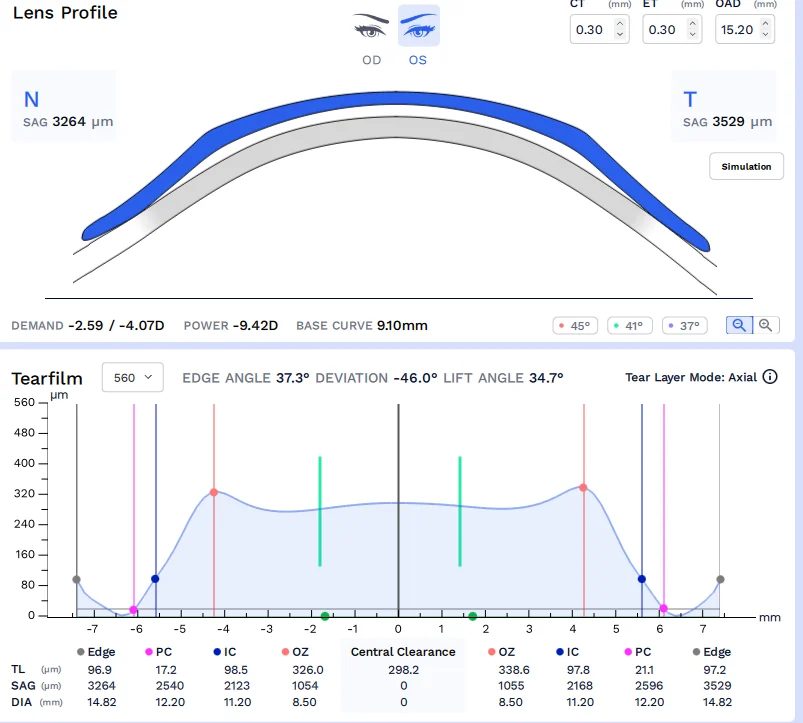
If you experience discomfort or irritation, remove the lenses and rinse your eyes with preservative-free saline solution. Contact your eye care professional for further guidance and evaluation. Adjustments to the fit or prescription may be necessary for optimal comfort.













San Diego Vision Care Optometry provides advanced eye care, from routine exams to treating glaucoma, cataracts, and vision issues. Dr. Bruce Nguyen and Dr. Charles Tu are dedicated to ensuring lifelong visual health for all patients.